Psychedelic Therapy:
The Next Mental Health Revolution
How substances like psilocybin and ketamine are being used to treat depression and PTSD safely
For decades, mental health treatment has followed a familiar script: diagnose, prescribe a daily pill, and wait weeks or months for relief that may never fully arrive. For the 40 million Americans living with anxiety disorders and the millions more battling treatment-resistant depression and PTSD, this approach has often felt like swimming against an endless tide. But a seismic shift is underway. Groundbreaking research into psychedelic-assisted therapy is rewriting the rules of mental healthcare, offering hope where conventional treatments have failed. This is not about recreational drug use. This is about science, safety, and a new frontier in healing the human mind.
The Science of Psychedelic Healing
Psychedelic therapy represents a paradigm shift in how we understand and treat mental illness. Unlike traditional antidepressants that require daily dosing and work by gradually adjusting neurotransmitter levels, psychedelics like psilocybin and ketamine work through fundamentally different mechanisms. They do not just mask symptoms; they appear to help the brain rewire itself.
At the heart of this revolution is a concept called neuroplasticity the brain’s ability to form new neural connections and reorganize itself. Research published in leading journals suggests that psychedelics promote this process by increasing levels of brain-derived neurotrophic factor (BDNF), a protein essential for the growth and maintenance of neurons. In practical terms, this means the brain becomes more flexible, more adaptable, and better able to process trauma, break negative thought patterns, and form healthier cognitive pathways.

A landmark systematic review and meta-analysis published in The BMJ examined the efficacy of psilocybin for treating symptoms of depression across seven clinical trials involving 436 participants. The findings were striking: psilocybin treatment showed significant improvement in depression scores compared to control groups, with greater effectiveness observed among patients with secondary depression and those who had used psychedelics in the past. The standardized mean difference favored psilocybin intervention across all measured outcomes, providing robust evidence for its therapeutic potential.
Psilocybin: The Mushroom Medicine
Psilocybin has emerged as one of the most promising compounds in the psychedelic therapy landscape. Johns Hopkins Medicine has been at the forefront of this research, with their Center for Psychedelic and Consciousness Research conducting pioneering studies that have reshaped the scientific conversation around these substances. Their research has demonstrated that a single dose of psilocybin, administered in a controlled clinical setting with professional psychological support, can produce lasting reductions in depression and anxiety symptoms.

What makes psilocybin particularly compelling is the speed and durability of its effects. Traditional SSRIs often take four to six weeks to show any benefit, and many patients experience only partial relief. In contrast, psilocybin-assisted therapy typically involves just one to three sessions, with effects that can last for months. The experience itself, often described as profoundly meaningful by participants, appears to catalyze deep psychological processing that continues to unfold long after the substance has left the body.
The therapeutic model is critical here. Psilocybin is never administered as a standalone treatment. Patients undergo thorough screening and preparation, receive the compound in a comfortable, supervised environment with trained therapists present, and engage in integration sessions afterward to process their experience. This structured approach ensures safety and maximizes therapeutic outcomes.
🍄 How Psilocybin Therapy Works
- Preparation Phase: Comprehensive medical and psychological screening, followed by preparatory sessions to build trust and set intentions
- Medicine Session: Administered in a comfortable, controlled setting with eye shades and curated music, supervised by two trained therapists
- Integration Phase: Follow-up sessions to process insights, translate experiences into lasting behavioral changes, and provide ongoing support
- Duration: The acute psychedelic experience lasts 4-6 hours, but therapeutic benefits can persist for 6-12 months or longer
- Dosing: Typically 10-25mg of synthetic psilocybin, carefully calibrated to the individual’s body weight and psychological readiness
Ketamine: From Anesthetic to Antidepressant
While psilocybin remains in clinical trials, ketamine has already broken through to mainstream psychiatric practice. Originally developed as an anesthetic in the 1960s, ketamine has been repurposed as a rapid-acting antidepressant and is now available at specialized clinics across the United States. Its mechanism is distinct from both traditional antidepressants and classic psychedelics, it works primarily as an NMDA receptor antagonist, modulating glutamate, the brain’s most abundant excitatory neurotransmitter.
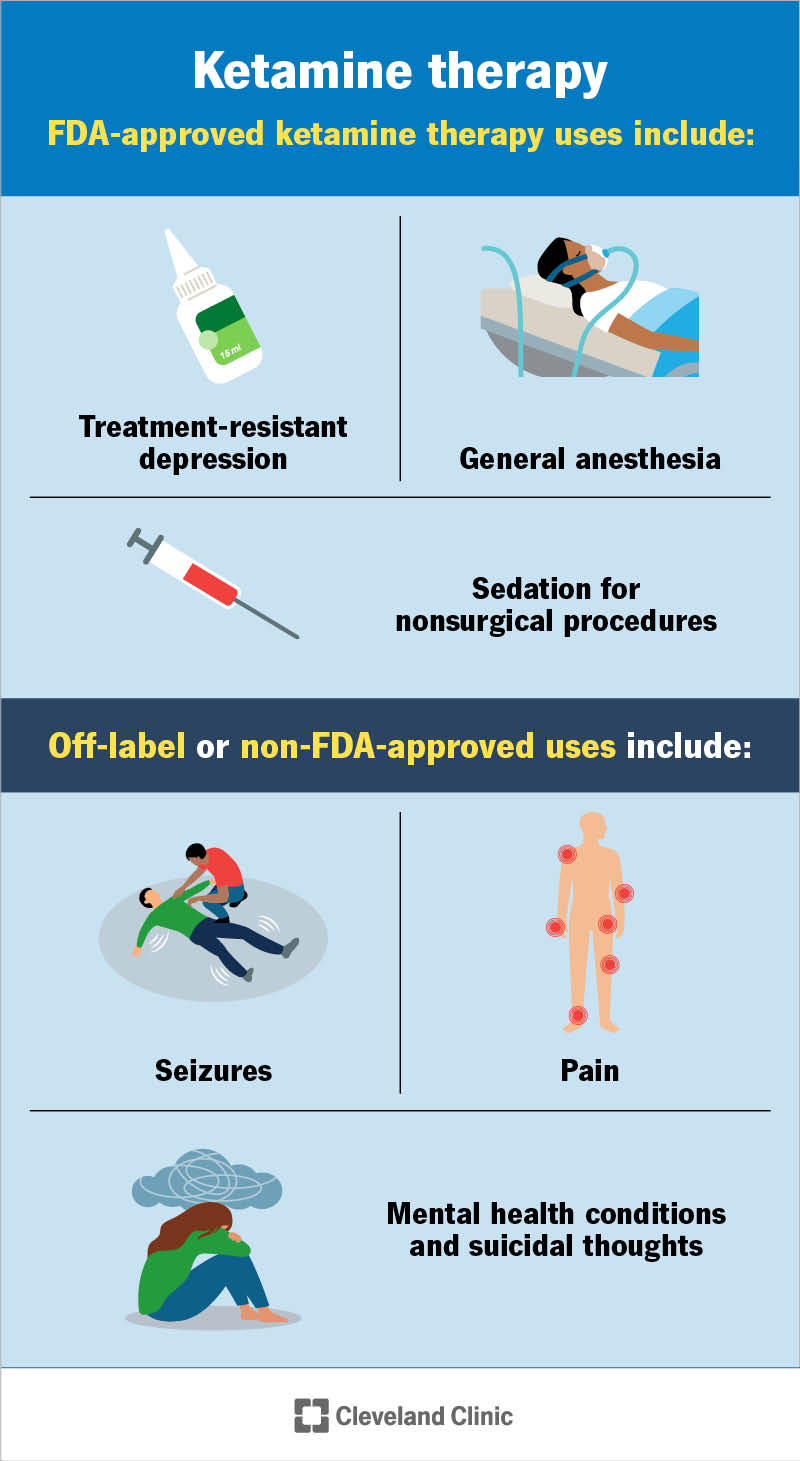
The evidence for ketamine’s efficacy in treating PTSD is particularly strong. A comprehensive systematic review and meta-analysis published in PubMed Central examined ten studies including five randomized controlled trials and found that ketamine demonstrated significant improvements in PTSD symptom severity. Improvements were noticeable both 24 hours after the first infusion and at the conclusion of treatment courses lasting one to four weeks. The analysis revealed a statistically significant effect for ketamine at the treatment endpoint, with the most common side effects being dose-related dissociative symptoms that typically peaked 40 minutes post-infusion and subsided within two hours.
One of the most groundbreaking studies was a randomized clinical trial conducted at the Icahn School of Medicine at Mount Sinai. Researchers found that a single intravenous infusion of ketamine (0.5 mg/kg) was associated with a significant and rapid reduction in PTSD symptom severity compared to midazolam, an active placebo control. The mean difference in Impact of Event Scale-Revised scores was 12.7 points 24 hours after infusion, a clinically meaningful improvement. Greater reduction of PTSD symptoms remained significant even after adjusting for baseline and 24-hour depressive symptom severity.
Ketamine holds promise as an effective treatment option for PTSD, particularly when paired with various psychotherapy approaches. The rapid onset of symptom relief represents a paradigm shift for patients who have suffered for years without adequate treatment.Systematic Review and Meta-Analysis, PubMed Central
Ketamine clinics are now popping up across the country, offering intravenous infusions, intranasal esketamine (Spravato, which is FDA-approved for treatment-resistant depression), and ketamine-assisted psychotherapy. The Cleveland Clinic provides comprehensive ketamine therapy programs that include treatment-resistant depression protocols, with patients typically receiving a series of six infusions over two to three weeks, followed by maintenance sessions as needed.

The FDA Fast-Track: A New Era of Approval
The regulatory landscape for psychedelic therapy has shifted dramatically. In April 2026, President Trump issued an Executive Order directing the U.S. Department of Health and Human Services to accelerate access to treatments for patients with serious mental illness. The FDA responded with a series of groundbreaking regulatory actions that signal a new era of acceptance for these therapies.
The FDA announced it is issuing National Priority Vouchers to three companies studying psychedelic compounds: two psilocybin compounds for treatment-resistant depression and major depressive disorder, and methylone (a compound similar to MDMA) for post-traumatic stress disorder. Each of these had previously received Breakthrough Therapy designation, which the FDA awards to therapies for serious conditions that demonstrate substantial improvement over currently available treatments.
In a significant first, the FDA also allowed an early-phase clinical study of noribogaine hydrochloride, a derivative of ibogaine, to move forward in the United States. This compound is being investigated as a potential treatment for alcohol use disorder, a condition with high relapse rates and desperately limited treatment options. The agency also announced it intends to release final guidance imminently to provide recommendations to sponsors developing serotonin-2A agonists and related products.
⚡ FDA 2026 Acceleration Actions
- Psilocybin (TRD): National Priority Voucher for treatment-resistant depression
- Psilocybin (MDD): National Priority Voucher for major depressive disorder
- Methylone: Priority Voucher for PTSD treatment
- Noribogaine: First-ever U.S. clinical study of an ibogaine derivative for alcohol use disorder
- Final Guidance: Imminent release for clinical trial design of serotonin-2A agonists
Health and Human Services Secretary Robert F. Kennedy Jr. stated: “Under President Trump’s leadership, we are accelerating the research, approval, and responsible access to promising mental health treatments including psychedelic therapies like ibogaine to confront our nation’s mental health crisis head-on, especially for our veterans.” FDA Commissioner Marty Makary, M.D., M.P.H. added: “These medications have the potential to address the nation’s mental health crisis, including conditions like treatment-resistant depression, alcoholism and other serious mental health and substance abuse conditions.”
Safety, Set, and Setting
The phrase “set and setting” coined by psychedelic pioneer Timothy Leary in the 1960s remains the cornerstone of safe psychedelic therapy today. “Set” refers to the patient’s mindset: their expectations, emotional state, and psychological preparation. “Setting” refers to the physical and social environment in which the experience occurs. Modern psychedelic therapy has elevated these principles into rigorous clinical protocols that prioritize patient safety above all else.

Contraindications are carefully screened. Patients with a personal or family history of psychotic disorders, such as schizophrenia or bipolar disorder with psychotic features, are typically excluded from psychedelic trials due to the risk of triggering latent psychosis. Cardiovascular screening is essential, as psilocybin can cause temporary increases in blood pressure and heart rate. Pregnancy, severe liver disease, and certain medications may also preclude participation.
During the session itself, patients are never left alone. Two trained therapists or guides remain present throughout, providing emotional support without directing the experience. The environment is designed to be comfortable, aesthetically pleasing, and free from distractions. Eye shades help patients turn their attention inward, while carefully curated music playlists often classical or ambient support the emotional journey. This container of safety allows patients to explore difficult emotions and memories that might otherwise be overwhelming.
The data on safety is reassuring. In the ketamine meta-analysis, no psychotic or manic symptoms were observed during treatment, and exposure to ketamine was not linked to an exacerbation of PTSD-related symptoms. Side effects were generally mild, transient, and well-tolerated. Similarly, Johns Hopkins research on psilocybin has demonstrated an excellent safety profile when administered in controlled clinical settings.
Who Can Benefit?
The potential applications of psychedelic therapy extend far beyond depression and PTSD. Research is actively exploring these compounds for alcohol use disorder, obsessive-compulsive disorder, end-of-life anxiety in terminal cancer patients, eating disorders, and even chronic pain. The common thread across these conditions is the presence of rigid, maladaptive thought patterns and emotional processing difficulties that psychedelics appear to help dissolve.
Treatment-resistant depression defined as depression that has not responded to at least two different antidepressant medications represents one of the most urgent unmet needs in psychiatry. For these patients, who may have suffered for years or even decades, psychedelic therapy offers a fundamentally different approach. Rather than incrementally adjusting brain chemistry, it creates a window of heightened neuroplasticity during which new perspectives and emotional insights can take root.
Veterans and first responders with PTSD represent another critical population. Traditional PTSD treatments, including SSRIs and trauma-focused psychotherapy, have remission rates that remain disappointingly low. The rapid-acting nature of ketamine and the profound psychological experiences facilitated by psilocybin may be particularly well-suited to addressing the deep-seated trauma that characterizes this condition. The FDA’s prioritization of these therapies for veteran populations reflects both the severity of the crisis and the strength of the emerging evidence.
The Road Ahead: Challenges and Opportunities
Despite the extraordinary promise, significant challenges remain. Access is limited, ketamine clinics are expensive and often not covered by insurance, while psilocybin and MDMA remain illegal outside of clinical trials. Training enough therapists to meet demand will require years of dedicated effort. And the medical establishment, while increasingly open, still harbors skepticism rooted in decades of stigma and misinformation.
There are also legitimate concerns about commercialization. As these therapies move toward mainstream acceptance, there is a risk that profit motives could compromise the careful, patient-centered approach that makes them effective. The psychedelic experience is not something that can be mass-produced or delivered via app. It requires time, presence, and genuine human connection. Maintaining these values as the field scales will be one of its greatest tests.
Research gaps persist as well. Most studies to date have been relatively small, and long-term data, while promising, remains limited. We need larger, more diverse trials that include underrepresented populations, as well as research into optimal dosing, frequency of sessions, and the role of different therapeutic modalities in conjunction with these medicines. The interaction between psychedelics and existing psychiatric medications also requires further investigation.

Yet the momentum is undeniable. From the halls of Johns Hopkins and NYU to the FDA and the White House, the conversation has shifted from “Should we study these substances?” to “How do we make them safely available to the people who need them most?” This is not a fringe movement anymore. It is mainstream medicine in the making.
A New Paradigm for Mental Health
Perhaps the most profound implication of psychedelic therapy is not any single compound or treatment protocol, but the paradigm shift it represents. For too long, psychiatry has treated the mind as a chemical machine to be tuned with daily pills. Psychedelic therapy suggests a different model: one that honors the complexity of human consciousness, the power of subjective experience, and the brain’s remarkable capacity for self-healing when given the right conditions.
This is not to say that psychedelics are a panacea. They will not replace all existing treatments, nor will they work for everyone. But for the millions of people who have tried everything and still suffer, they represent something that has been in desperately short supply: genuine hope. The kind of hope that comes not from marketing campaigns, but from rigorous science, compassionate care, and the lived experiences of people who have found relief after years of darkness.
As we stand at this inflection point, the path forward requires wisdom as much as enthusiasm. We must move quickly enough to help those suffering now, but carefully enough to preserve the integrity of these powerful medicines. We must make them accessible to all who need them, not just those who can afford premium clinic prices. And we must continue to ask hard questions, even as we celebrate the answers we’ve already found.
The mental health revolution is here. It is being led by scientists in lab coats, therapists in comfortable chairs, and patients brave enough to venture into the unknown territories of their own minds. It is being powered by compounds that humans have used for thousands of years, now refined and studied with the most sophisticated tools modern science can offer. And it is being guided by a growing recognition that healing is not just about managing symptoms, it is about transforming lives.
There is a growing recognition of the potential of psychedelic medications to address multiple different psychiatric conditions that are notoriously difficult to treat. At the FDA we are showing our support of investigating the safety and efficacy of this class of drugs.Tracy Beth Hoeg, M.D., Ph.D., Acting Director, FDA Center for Drug Evaluation and Research
Explore Further
Trusted resources and research institutions leading the psychedelic therapy revolution


